How Frozen Shoulder Occurs
Shoulder pain is a highly irritating ailment. It can prevent you from sleeping, participating in sport, and working comfortably. The problem with pain in the shoulder is that the joint is designed to provide flexible movement, so when it is sore there are many things you will be unable to do, such as reaching for items when shopping, washing your hair, or even holding the steering wheel of your car.
So, if you have shoulder pain, is it debilitating and stiff, occurring gradually for no reason? Are you struggling to sleep as a result of your shoulder pain? Do you also have diabetes, thyroid issues or a hormone imbalance? If so, you may have a frozen shoulder. Frozen shoulder, or adhesive capsulitis, is an issue that is highly irritable for the sufferer. What you may want to know is; how does frozen shoulder occur, and how do we treat it? We will answer the first question in this Blog and the second question in our follow-up Blog, “How can frozen shoulder be cured.”
Why is it called ‘’Frozen Shoulder’’?
Despite the way it sounds, the shoulder doesn’t feel cold, and it doesn’t occur by lying in the cold (which are two common myths I must undo when talking to patients about their shoulder pain). The condition was first described by S. Duplay in 1872, who called it ‘’periarthritis scapulohumeral’’. This became ‘’frozen shoulder’’ in 1934 when E. A. Codman, witnessed the a slow, painful shoulder condition that seemed to ‘’freeze up’’ in the sense of a lack of movement, rather than a temperature sense.
What is frozen shoulder?
Frozen shoulder is a condition where the shoulder joint succumbs to something known as arthrofibrosis, which is the result of excessive scar tissue or adhesions building up in the joint. This leads to stiffness, pain and dysfunction. The official definition is:
“A condition of uncertain aetiology, characterised by significant restriction of both active and passive shoulder motion that occurs in the absence of a known intrinsic shoulder disorder’’
What separates frozen shoulder from other shoulder ailments is that there is usually no specific reason for the pain. Sufferers will describe the symptoms as pain followed by a reduction in the range of movements of the shoulder. What makes this condition really interesting is the seeming lack of explanation for how, and what causes it to develop.
A typical frozen shoulder patient will be 55 years old, female, and could have other underlying conditions, such as:
- Autoimmune conditions
- Diabetes
- Over and underactive thyroid
- Tuberculosis
- Parkinson’s disease
- Previous injury to the shoulder
- Chest/breast surgery
How frozen shoulder occurs
Autoimmune conditions
An autoimmune condition is a condition where the body attacks itself. This, surprisingly, can be a major factor in the development of frozen shoulder. This may be because certain proteins (serum immunoglobulin) are reduced, which results in a hypersensitivity autoimmune reaction, causing inflammation.
Diabetes
Diabetes is a metabolic syndrome, which is a medical term for a combination of hypertension and obesity, alongside diabetes. The primary reason for this may be because someone who has a metabolic syndrome will have elevated hormones levels that are associated with inflammation. Another reason could be that as a result of consistently high blood sugar levels, your collagen becomes sticky, which can result in stiffness, alongside the regressive effects of dehydration caused by the elevated blood sugar levels.
Overactive and underactive thyroid
An overactive, or underactive, thyroid is an endocrine condition, which causes hormone imbalances among other problems. This change in hormones can result in inflammation and fibrosis, which is what causes the pain and stiffness.
Tuberculosis
Frozen shoulder can also occur alongside pulmonary tuberculosis. This could be a result of the lack of mobility present while suffering from tuberculosis.
Parkinson’s disease
Because Parkinson’s disease sufferers experience slowness in their movements as well as stiffness. Interestingly, sometimes symptoms of frozen shoulder can be one of the first noticeable symptoms that Parkinson’s disease sufferers experience. Furthermore, frozen shoulder is far more commonly seen at the onset of Parkinson’s disease and is rarely seen years into the disease.

Previous injury to the shoulder
Similar to the above, a previous injury can immobilise and stiffen the shoulder, which can cause frozen shoulder. Previous injuries may also create inflammation around the tissues, which can result in frozen shoulder.
Chest/breast surgery
Post-surgical immobilisation can result in the stiffness and a build-up of inflammation in the shoulder.
What are the different stages of the frozen shoulder?
For more details on the progressive stages and how to treat frozen shoulder, please refer to our Blog: “How frozen shoulder can be cured.” As a follow-up to this Blog, we will give you an overview into how it can be treated and cured.
There are three phases to frozen shoulder (image from Singapore Medical Association: https://pubmed.ncbi.nlm.nih.gov/29242941/).
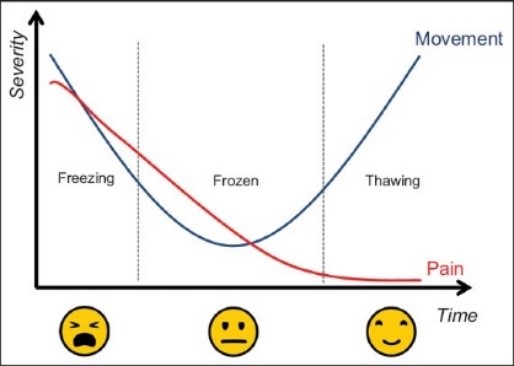
Phase 1:
This is known as the ‘painful phase’, or ‘freezing phase’. This is where both the pain and lack of movement are at a peak.
This phase could last in between month 2 and 9 from 2 to 9 months?. Symptoms you may experience may gradually increase to severe pain, which worsens at night.
Phase 2:
The frozen phase is similar to the freezing phase; it continues to be painful and stiff. This stage can be present for 4 to 12 months, and is recognisable because, although the pain begins to subside, the range of motion is progressively reduces. You will be able to increase exercise on the affected area, but good form is still very much encouraged not clear.
Phase 3:
The recovery phase is characterised by a gradual return of the range of motion. In this phase, it is important that we get the shoulder back to its’ normal range of motion as quickly as possible, because the shoulder will be a lot weaker due to the lack of movement over the previous months. During this phase, you have to push your shoulder further within the pain boundary.
What else do you need to know?
Now that we have explained in reasonable depth what frozen shoulder is, and how it occurs, you will need to know how to fix it. This is answered in our second blog which will explain the exercises, probable recovery timelines and any other information you may need to know when recovering from frozen shoulder.
For any further questions, please don’t hesitate to ask:
0161 209 2980
info@movementandwellbeingclinic.co.uk
Ed Madeley M.Ost
