How Frozen Shoulder is Cured
Intro
Shoulder pain continues to be a difficult area to treat for manual therapists. The shoulder joint is such a complex joint, partly because it is quite unstable. The bony contact of the glenohumeral joint (the ball and socket joint in the shoulder) is similar to a golf ball and tee, which suggests it isn’t very much! Frozen shoulder is no exception, but the purpose of this Blog is to show how it can be cured.
Due to the complex nature of frozen shoulder, we wrote a related Blog entitled How Frozen Shoulder Occurs. This detailed exactly how your frozen shoulder may have started, and what risk factors you may have that can lead to the condition. Because of the related blog, we will only give a brief reminder regarding this.

Definition: What is it?
Frozen shoulder is a condition that causes a lot of pain, stiffness, and dysfunction to the shoulder joint. It is a condition that is unusual for two main reasons.
The condition can commonly last for over 2 years, whereas most pain related conditions will either be intermittent, or they will be resolved in a matter of days, weeks or months.
The second unusual trait is that there seems to be no movement related reason for developing the condition. The main risk factors for developing frozen shoulder are:
- Autoimmune conditions
- Diabetes
- Over and underactive thyroid
- Tuberculosis
- Parkinson’s disease
- Previous injury to the shoulder
- Chest/breast surgery
Why is it important to get cured? Studies show that up to 20% of your range of shoulder moment may be lost if not treated. Since 90% of people recover without requiring surgery, fortunately, there are many conservative options. Below, we have analysed the data and given you a list of treatment options to aid your recovery from frozen shoulder.
What are my options?
Physical therapy
Joint mobilisation, carried out by Osteopaths and Physiotherapists has been shown to be the most effective treatment for frozen shoulder. It is important to note that this needs to be non-aggressive, especially in the first two stages of the condition. Exercise can keep the lubrication of the joint flowing, which can decrease pain, speed up recovery time and keep the range of motion as high as possible as the joint ‘freezes’.
Manual therapy
Manual therapy has a similar significant impact on range of motion, pain levels and recovery time. Moving the joint ‘actively’ (which involves the patient moving themselves in physical therapy) is great, but can be restrictive. Your Osteopath or Physiotherapist can mobilise your shoulder ‘passively’, which means that the patient relaxes and allows the therapist to move the arm for them. This works because frozen shoulder involves a hardening of the ligaments and joint capsule, so passive movement results in the elongation of the collagen, which is what the tissue is composed of. This works well combined with the active physical therapy. TENS machines can also help with mobilising the shoulder while the patient is relaxed, together with physical therapy and manual therapy.

Soft tissue mobilisation
There is some research that shows positive results from massage therapy treatment. Massage therapy can help with pain relief and reduce scar tissue in the area. Soft tissue work on the area has been shown to help with the stimulation of the collagen fibres, as well as an improvement in circulation around the joint.
Taping
Taping may be helpful in reducing pain and helping with postural cues/cures?. This may help, since poor posture can exacerbate frozen shoulder, but patients with frozen shoulder also need a cure for scapula winging (otherwise known as scapula dyskinesia). It is important to note that there is no current research on this issue that has been published.
Injections
Injections into the shoulder joint can also be helpful. There are a variety of options, including a steroid to reduce the inflammation, an aesthetic to reduce the pain and a saline solution to expand and stretch the joint capsule.
Surgery
If all of the above interventions fail, an arthroscopic release and manipulation under anaesthetic is the next step. This involves a keyhole surgery procedure to release the ligaments under the joint, and then mobilising the joint during anaesthetic.
Rehab plan
As discussed, the evidence shows that exercise combined with manual therapy is the most effective method in curing frozen shoulder. Here is a breakdown of the three stages, and recommended treatment to cure your frozen shoulder.
Freezing phase
The freezing phase is also known as the ‘painful phase’, and is associated with a lack of movement and extreme pain.
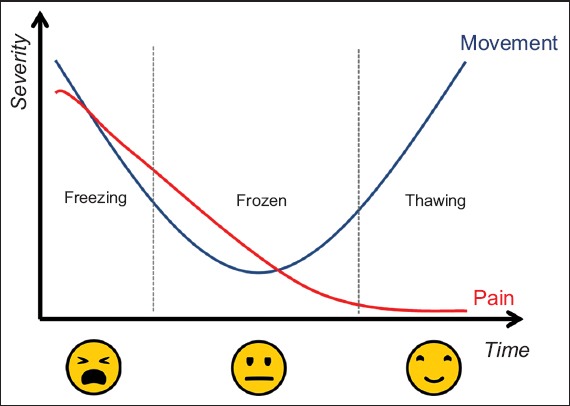
This phase could last in between months 2 and 9. Symptoms you may experience are a gradual increase in severe pain which worsens at night.
If you’re suffering from this phase, what can help is Osteopathy techniques, such as traction & mobilisation, pain relieving exercises and heat or ice packs. Another treatment technique can be the use of moist heat combined with with stretching and other physical therapy. Examples of the physical therapy exercises include:
- Gentle shoulder mobilisation (pendulum exercises, passive stretching)
- Active shoulder mobilisation (rotation, circumduction)
- Self-traction techniques
- Pulling exercises to improve posture
These exercises should be performed for 3 sets of around 1-5 seconds within a range of motion that doesn’t cause pain.
Frozen phase
The frozen phase is still painful and stiff and can last from 4 to 12 months. In this phase expect the pain to subside. It is important that if you’re in this phase, you should try and push the limits of what you’re capable of doing, remembering good form.
Remember osteopathy techniques help supplement the exercise rehab plan. Examples of exercises is this stage are:
- Shoulder blade retraction (bringing the shoulder blades together)
- Posterior capsule stretch (like you’re giving yourself a hug)
- Shoulder internal rotation
- Assisted external rotation with a wand
These exercises should be performed for 3 sets, adding more time than the freezing phase – aim for 15-20 seconds.
Thawing phase
The thawing phase is where you will experience a gradual improvement in the range of motion. One issue with the shoulder in this phase is that there will be a significant loss in strength, so regaining mobility and strength is the number one goal from this phase. Because of this, we need to push the exercises more which will encourage a little pain.
This phase requires a longer hold duration, and will also involve movement exercises as well as eventually free weights. It is important to set a pain boundary that you are willing/able to tolerate, as although we need to push through the pain, we don’t want to overdo it. Exercises include:
- Banded eccentric external rotations
- Lateral raises to 45 degrees
- Sidelying external rotations with free-weights
- Shoulder press
For any further questions, please don’t hesitate to ask:
0161 209 2980
info@movementandwellbeingclinic.co.uk
Ed Madeley M.Ost